Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
- Triglyceride-Glucose Index Predicts Future Atherosclerotic Cardiovascular Diseases: A 16-Year Follow-up in a Prospective, Community-Dwelling Cohort Study
- Joon Ho Moon, Yongkang Kim, Tae Jung Oh, Jae Hoon Moon, Soo Heon Kwak, Kyong Soo Park, Hak Chul Jang, Sung Hee Choi, Nam H. Cho
- Endocrinol Metab. 2023;38(4):406-417. Published online August 3, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1703
- 2,674 View
- 166 Download
- 3 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
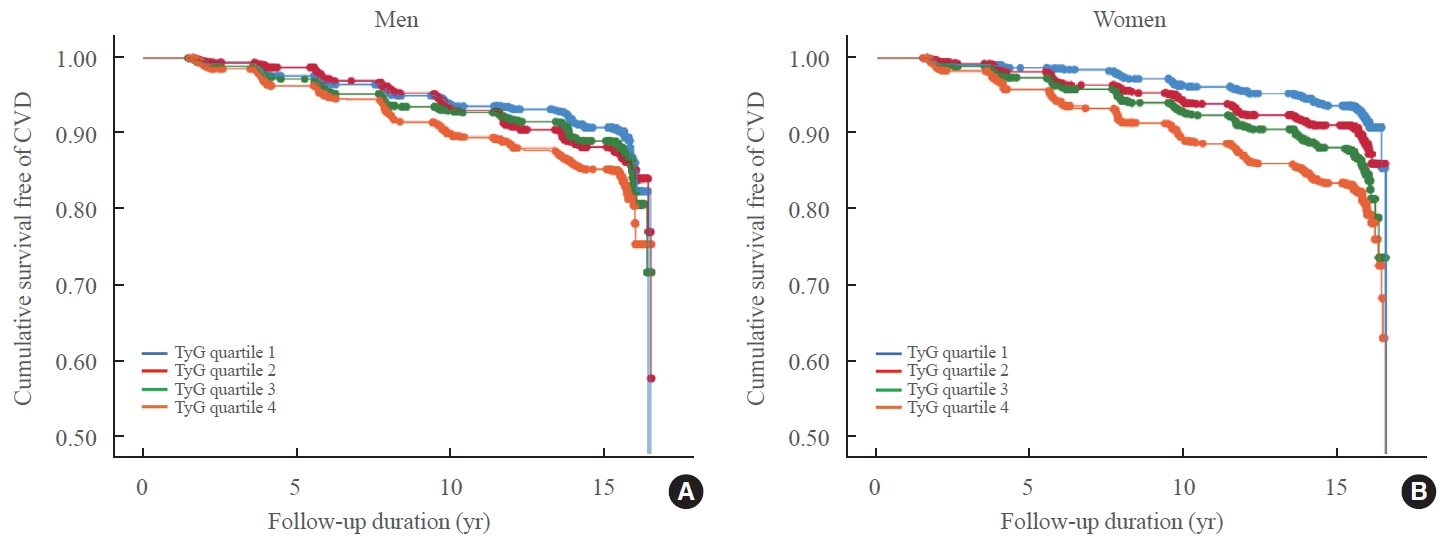
While the triglyceride-glucose (TyG) index is a measure of insulin resistance, its association with cardiovascular disease (CVD) has not been well elucidated. We evaluated the TyG index for prediction of CVDs in a prospective large communitybased cohort.
Methods
Individuals 40 to 70 years old were prospectively followed for a median 15.6 years. The TyG index was calculated as the Ln [fasting triglycerides (mg/dL)×fasting glucose (mg/dL)/2]. CVDs included any acute myocardial infarction, coronary artery disease or cerebrovascular disease. We used a Cox proportional hazards model to estimate CVD risks according to quartiles of the TyG index and plotted the receiver operating characteristics curve for the incident CVD.
Results
Among 8,511 subjects (age 51.9±8.8 years; 47.5% males), 931 (10.9%) had incident CVDs during the follow-up. After adjustment for age, sex, body mass index, diabetes mellitus, hypertension, total cholesterol, smoking, alcohol, exercise, and C-reactive protein, subjects in the highest TyG quartile had 36% increased risk of incident CVD compared with the lowest TyG quartile (hazard ratio, 1.36; 95% confidence interval, 1.10 to 1.68). Carotid plaque, assessed by ultrasonography was more frequent in subjects in the higher quartile of TyG index (P for trend=0.049 in men and P for trend <0.001 in women). The TyG index had a higher predictive power for CVDs than the homeostasis model assessment of insulin resistance (HOMA-IR) (area under the curve, 0.578 for TyG and 0.543 for HOMA-IR). Adding TyG index on diabetes or hypertension alone gave sounder predictability for CVDs.
Conclusion
The TyG index is independently associated with future CVDs in 16 years of follow-up in large, prospective Korean cohort. -
Citations
Citations to this article as recorded by- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus
Kaisheng Yuan, Bing Wu, Ruiqi Zeng, Fuqing Zhou, Ruixiang Hu, Cunchuan Wang
Diabetes, Obesity and Metabolism.2024; 26(1): 169. CrossRef - Association between the triglyceride glucose index and chronic total coronary occlusion: A cross-sectional study from southwest China
Kaiyong Xiao, Huili Cao, Bin Yang, Zhe Xv, Lian Xiao, Jianping Wang, Shuiqing Ni, Hui Feng, Zhongwei He, Lei Xv, Juan Li, Dongmei Xv
Nutrition, Metabolism and Cardiovascular Diseases.2024; 34(4): 850. CrossRef - The association between TyG and all-cause/non-cardiovascular mortality in general patients with type 2 diabetes mellitus is modified by age: results from the cohort study of NHANES 1999–2018
Younan Yao, Bo Wang, Tian Geng, Jiyan Chen, Wan Chen, Liwen Li
Cardiovascular Diabetology.2024;[Epub] CrossRef - Triglyceride-glucose index predicts type 2 diabetes mellitus more effectively than oral glucose tolerance test-derived insulin sensitivity and secretion markers
Min Jin Lee, Ji Hyun Bae, Ah Reum Khang, Dongwon Yi, Mi Sook Yun, Yang Ho Kang
Diabetes Research and Clinical Practice.2024; 210: 111640. CrossRef - Evaluation of the novel three lipid indices for predicting five- and ten-year incidence of cardiovascular disease: findings from Kerman coronary artery disease risk factors study (KERCADRS)
Alireza Jafari, Hamid Najafipour, Mitra Shadkam, Sina Aminizadeh
Lipids in Health and Disease.2023;[Epub] CrossRef
- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus

- Diabetes, Obesity and Metabolism
- Effect of the Concomitant Use of Subcutaneous Basal Insulin and Intravenous Insulin Infusion in the Treatment of Severe Hyperglycemic Patients
- Yejee Lim, Jung Hun Ohn, Joo Jeong, Jiwon Ryu, Sun-wook Kim, Jae Ho Cho, Hee-Sun Park, Hye Won Kim, Jongchan Lee, Eun Sun Kim, Nak-Hyun Kim, You Hwan Jo, Hak Chul Jang
- Endocrinol Metab. 2022;37(3):444-454. Published online June 3, 2022
- DOI: https://doi.org/10.3803/EnM.2021.1341
- 59,030 View
- 240 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
No consensus exists regarding the early use of subcutaneous (SC) basal insulin facilitating the transition from continuous intravenous insulin infusion (CIII) to multiple SC insulin injections in patients with severe hyperglycemia other than diabetic ketoacidosis. This study evaluated the effect of early co-administration of SC basal insulin with CIII on glucose control in patients with severe hyperglycemia.
Methods
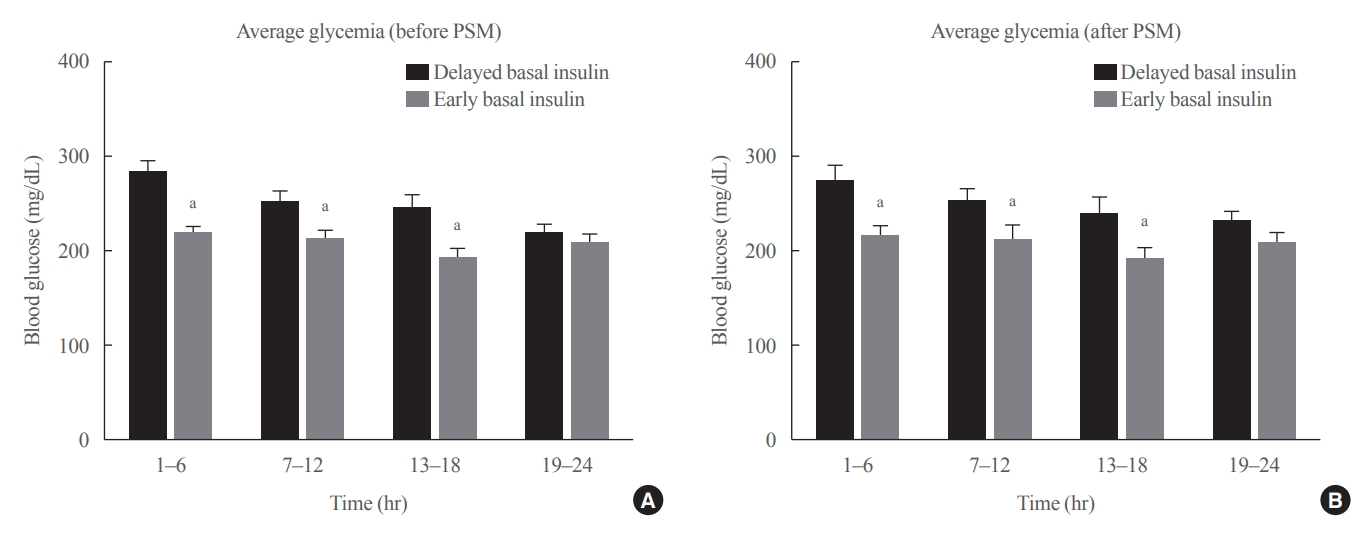
Patients who received CIII for the management of severe hyperglycemia were divided into two groups: the early basal insulin group (n=86) if they received the first SC basal insulin 0.25 U/kg body weight within 24 hours of CIII initiation and ≥4 hours before discontinuation, and the delayed basal insulin group (n=79) if they were not classified as the early basal insulin group. Rebound hyperglycemia was defined as blood glucose level of >250 mg/dL in 24 hours following CIII discontinuation. Propensity score matching (PSM) methods were additionally employed for adjusting the confounding factors (n=108).
Results
The rebound hyperglycemia incidence was significantly lower in the early basal insulin group than in the delayed basal insulin group (54.7% vs. 86.1%), despite using PSM methods (51.9%, 85.2%). The length of hospital stay was shorter in the early basal insulin group than in the delayed basal insulin group (8.5 days vs. 9.6 days, P=0.027). The hypoglycemia incidence did not differ between the groups.
Conclusion
Early co-administration of basal insulin with CIII prevents rebound hyperglycemia and shorten hospital stay without increasing the hypoglycemic events in patients with severe hyperglycemia. -
Citations
Citations to this article as recorded by- 16. Diabetes Care in the Hospital: Standards of Care in Diabetes—2024
Nuha A. ElSayed, Grazia Aleppo, Raveendhara R. Bannuru, Dennis Bruemmer, Billy S. Collins, Laya Ekhlaspour, Rodolfo J. Galindo, Marisa E. Hilliard, Eric L. Johnson, Kamlesh Khunti, Ildiko Lingvay, Glenn Matfin, Rozalina G. McCoy, Mary Lou Perry, Scott J.
Diabetes Care.2024; 47(Supplement): S295. CrossRef - 16. Diabetes Care in the Hospital: Standards of Care in Diabetes—2023
Nuha A. ElSayed, Grazia Aleppo, Vanita R. Aroda, Raveendhara R. Bannuru, Florence M. Brown, Dennis Bruemmer, Billy S. Collins, Marisa E. Hilliard, Diana Isaacs, Eric L. Johnson, Scott Kahan, Kamlesh Khunti, Jose Leon, Sarah K. Lyons, Mary Lou Perry, Priya
Diabetes Care.2023; 46(Supplement): S267. CrossRef - Effectiveness and safety of early insulin glargine administration in combination with continuous intravenous insulin infusion in the management of diabetic ketoacidosis: A randomized controlled trial
Kitti Thammakosol, Chutintorn Sriphrapradang
Diabetes, Obesity and Metabolism.2023; 25(3): 815. CrossRef
- 16. Diabetes Care in the Hospital: Standards of Care in Diabetes—2024

- Diabetes, Obesity and Metabolism
- The Effects of PPAR Agonists on Atherosclerosis and Nonalcoholic Fatty Liver Disease in ApoE−/−FXR−/− Mice
- Yenna Lee, Bo-Rahm Kim, Geun-Hyung Kang, Gwan Jae Lee, Young Joo Park, Haeryoung Kim, Hak Chul Jang, Sung Hee Choi
- Endocrinol Metab. 2021;36(6):1243-1253. Published online December 28, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1100
- 5,619 View
- 159 Download
- 11 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Farnesoid X receptor (FXR), a bile acid–activated nuclear receptor, is a potent regulator of glucose and lipid metabolism as well as of bile acid metabolism. Previous studies have demonstrated that FXR deficiency is associated with metabolic derangements, including atherosclerosis and nonalcoholic fatty liver disease (NAFLD), but its mechanism remains unclear. In this study, we investigated the role of FXR in atherosclerosis and NAFLD and the effect of peroxisome proliferator-activated receptor (PPAR) agonists in mouse models with FXR deficiency.
Methods
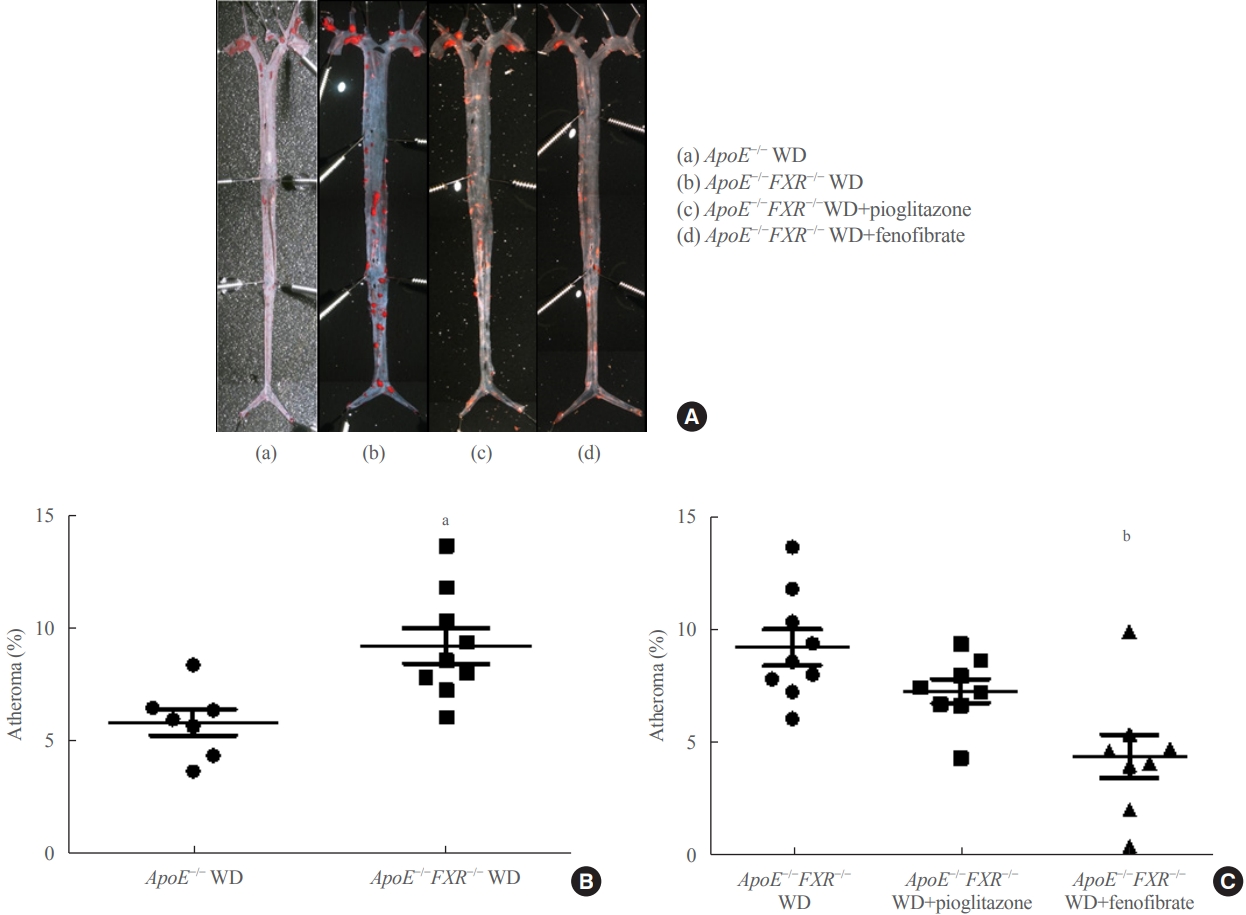
En face lipid accumulation analysis, liver histology, serum levels of glucose and lipids, and mRNA expression of genes related to lipid metabolism were compared between apolipoprotein E (ApoE)−/− and ApoE−/−FXR−/− mice. The effects of PPARα and PPARγ agonists were also compared in both groups of mice.
Results
Compared with ApoE−/− mice, ApoE−/−FXR−/− mice showed more severe atherosclerosis, hepatic steatosis, and higher levels of serum cholesterol, low-density lipoprotein cholesterol, and triglycerides, accompanied by increased mRNA expression of FAS, ApoC2, TNFα, IL-6 (liver), ATGL, TGH, HSL, and MGL (adipocytes), and decreased mRNA expressions of CPT2 (liver) and Tfam (skeletal muscle). Treatment with a PPARα agonist, but not with a PPARγ agonist, partly reversed atherosclerosis and hepatic steatosis, and decreased plasma triglyceride levels in the ApoE−/−FXR−/− mice, in association with increased mRNA expression of CD36 and FATP and decreased expression of ApoC2 and ApoC3 (liver).
Conclusion
Loss of FXR is associated with aggravation of atherosclerosis and hepatic steatosis in ApoE-deficient mice, which could be reversed by a PPARα agonist through induction of fatty acid uptake, β-oxidation, and triglyceride hydrolysis. -
Citations
Citations to this article as recorded by- Evaluation of the hepatotoxicity of Psoralea corylifolia L. based on a zebrafish model
Shu-Yan Gao, Jing-Cheng Zhao, Qing Xia, Chen Sun, Maimaiti Aili, Ainiwaer Talifu, Shi-Xia Huo, Yun Zhang, Zhi-Jian Li
Frontiers in Pharmacology.2024;[Epub] CrossRef - Advances in management of metabolic dysfunction-associated steatotic liver disease: from mechanisms to therapeutics
Yuxiao Jiang, Lili Wu, Xiaopeng Zhu, Hua Bian, Xin Gao, Mingfeng Xia
Lipids in Health and Disease.2024;[Epub] CrossRef - Mitochondrial carnitine palmitoyltransferase-II dysfunction: A possible novel mechanism for nonalcoholic fatty liver disease in hepatocarcinogenesis
Min Yao, Ping Zhou, Yan-Yan Qin, Li Wang, Deng-Fu Yao
World Journal of Gastroenterology.2023; 29(12): 1765. CrossRef - Emerging Roles of Gut Microbial Modulation of Bile Acid Composition in the Etiology of Cardiovascular Diseases
Tess Yntema, Debby P. Y. Koonen, Folkert Kuipers
Nutrients.2023; 15(8): 1850. CrossRef - The interplay between nonalcoholic fatty liver disease and atherosclerotic cardiovascular disease
Alexandra C. Finney, Sandeep Das, Dhananjay Kumar, M. Peyton McKinney, Bishuang Cai, Arif Yurdagul, Oren Rom
Frontiers in Cardiovascular Medicine.2023;[Epub] CrossRef - Targeting PPARs for therapy of atherosclerosis: A review
Miao Miao, Xue Wang, Tian Liu, Yan-Jie Li, Wen-Qian Yu, Tong-Mei Yang, Shou-Dong Guo
International Journal of Biological Macromolecules.2023; 242: 125008. CrossRef - Cabernet sauvignon dry red wine ameliorates atherosclerosis in mice by regulating inflammation and endothelial function, activating AMPK phosphorylation, and modulating gut microbiota
Xinlong Cheng, Xue Han, Liangfu Zhou, Yasai Sun, Qian Zhou, Xuan Lin, Zhe Gao, Jie Wang, Wen Zhao
Food Research International.2023; 169: 112942. CrossRef - Impacts of dietary lipids derived from animal or vegetable sources on healthy rats
Mostafa M Dalal, Gamal M Edrees, Hanaa A Hassan, Mamdouh Abdel-Mogib, Mai Alaa El-Dein
Egyptian Journal of Basic and Applied Sciences.2023; 10(1): 618. CrossRef - Whey protein hydrolysate alleviated atherosclerosis and hepatic steatosis by regulating lipid metabolism in apoE-/- mice fed a Western diet
Kai Wang, Zixin Fu, Xiaoyi Li, Hui Hong, Xin Zhan, Xiaohong Guo, Yongkang Luo, Yuqing Tan
Food Research International.2022; 157: 111419. CrossRef - Melatonin alleviates PM2.5‐induced glucose metabolism disorder and lipidome alteration by regulating endoplasmic reticulum stress
Zhou Du, Junjie Hu, Lisen Lin, Qingqing Liang, Mengqi Sun, Zhiwei Sun, Junchao Duan
Journal of Pineal Research.2022;[Epub] CrossRef - Lipoprotein Lipase: Is It a Magic Target for the Treatment of Hypertriglyceridemia
Joon Ho Moon, Kyuho Kim, Sung Hee Choi
Endocrinology and Metabolism.2022; 37(4): 575. CrossRef - The role of the gut microbiota in health and cardiovascular diseases
Lu Wang, Shiqi Wang, Qing Zhang, Chengqi He, Chenying Fu, Quan Wei
Molecular Biomedicine.2022;[Epub] CrossRef
- Evaluation of the hepatotoxicity of Psoralea corylifolia L. based on a zebrafish model

- Clinical Study
- Longitudinal Changes of High Molecular Weight Adiponectin are Associated with Postpartum Development of Type 2 Diabetes Mellitus in Patients with Gestational Diabetes Mellitus
- Dong-Hwa Lee, Jung Ah Lim, Jung Hee Kim, Soo Heon Kwak, Sung Hee Choi, Hak Chul Jang
- Endocrinol Metab. 2021;36(1):114-122. Published online February 24, 2021
- DOI: https://doi.org/10.3803/EnM.2020.831
- 3,931 View
- 104 Download
- 4 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The influence of serial changes of adipokines on maternal glucose metabolism from pregnancy to postpartum periods in women with previous gestational diabetes mellitus (pGDM) has not been thoroughly explored. We tried to examine the relationship between the serial changes of adipokines and the development of diabetes mellitus (DM) in women with pGDM.
Methods
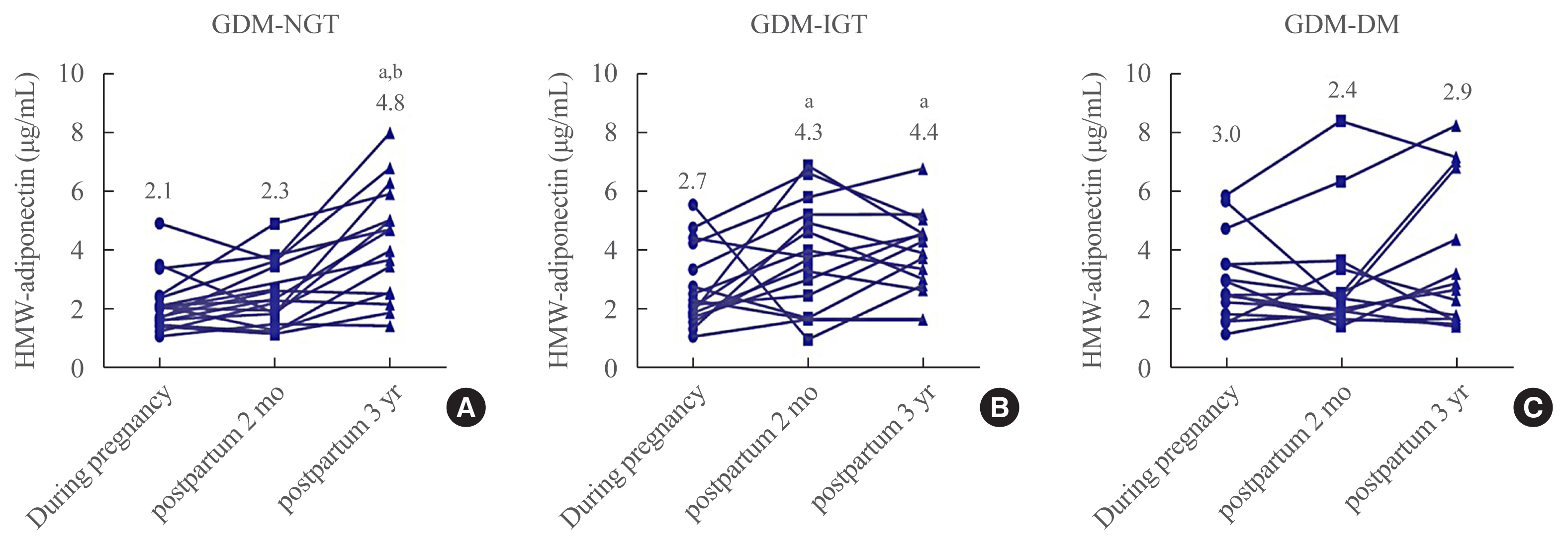
We longitudinally measured following adipokines: high molecular weight (HMW) adiponectin, retinol-binding protein-4 (RBP-4), lipocalin-2, and chemerin, during pregnancy, and at 2 months and 3 years after delivery. Based on glucose status at postpartum 3 years, we divided into three groups: normal glucose tolerance (GDM-NGT, n=20), impaired glucose tolerance (GDM-IGT, n=23), and GDM-DM (n=22). We analyzed the correlations between adipokines and various metabolic parameters.
Results
Plasma HMW adiponectin levels were not different among the three groups during pregnancy. However, HMW adiponectin levels increased at 3 years after the delivery in women with GDM-NGT compared with women with GDM-DM. In the GDM-IGT group, HMW adiponectin levels increased at 2 months postpartum compared to pregnancy period. In contrast, HMW adiponectin levels showed no alternation after parturition in women with GDM-DM. HMW adiponectin was negatively correlated with body mass index and a homeostasis model assessment of insulin resistance. Other adipokines such as RBP-4, lipocalin-2, and chemerin neither showed any differences among the groups nor any significant correlations with 3 years postpartum status of glucose intolerance.
Conclusion
Serial changes of HMW adiponectin are associated with the maintenance of glucose metabolism in women with pGDM after delivery. -
Citations
Citations to this article as recorded by- Reproductive risk factors across the female lifecourse and later metabolic health
Amy R. Nichols, Jorge E. Chavarro, Emily Oken
Cell Metabolism.2024; 36(2): 240. CrossRef - Gestational Diabetes Mellitus and Colostral Appetite-Regulating Adipokines
Jolanta Lis-Kuberka, Marta Berghausen-Mazur, Magdalena Orczyk-Pawiłowicz
International Journal of Molecular Sciences.2024; 25(7): 3853. CrossRef - The levels of osteopontin in human milk of Chinese mothers and its associations with maternal body composition
Huijuan Ruan, Qingya Tang, Xuan Zhao, Yajie Zhang, Xuelin Zhao, Yi Xiang, Wei Geng, Yi Feng, Wei Cai
Food Science and Human Wellness.2022; 11(5): 1419. CrossRef - Association of circulatory adiponectin with the parameters of Madras Diabetes Research Foundation-Indian Diabetes Risk Score
MohdD Khan, MohammadK Ahmad, Roshan Alam, Saba Khan, Geeta Jaiswal, MohammadM Khan
Journal of Diabetology.2022; 13(4): 331. CrossRef
- Reproductive risk factors across the female lifecourse and later metabolic health

- Thyroid
- Validity and Reliability of the Korean Version of the Hyperthyroidism Symptom Scale
- Jie-Eun Lee, Dong Hwa Lee, Tae Jung Oh, Kyoung Min Kim, Sung Hee Choi, Soo Lim, Young Joo Park, Do Joon Park, Hak Chul Jang, Jae Hoon Moon
- Endocrinol Metab. 2018;33(1):70-78. Published online March 21, 2018
- DOI: https://doi.org/10.3803/EnM.2018.33.1.70
- 4,048 View
- 55 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Background Thyrotoxicosis is a common disease resulting from an excess of thyroid hormones, which affects many organ systems. The clinical symptoms and signs are relatively nonspecific and can vary depending on age, sex, comorbidities, and the duration and cause of the disease. Several symptom rating scales have been developed in an attempt to assess these symptoms objectively and have been applied to diagnosis or to evaluation of the response to treatment. The aim of this study was to assess the reliability and validity of the Korean version of the hyperthyroidism symptom scale (K-HSS).
Methods Twenty-eight thyrotoxic patients and 10 healthy subjects completed the K-HSS at baseline and after follow-up at Seoul National University Bundang Hospital. The correlation between K-HSS scores and thyroid function was analyzed. K-HSS scores were compared between baseline and follow-up in patient and control groups. Cronbach's α coefficient was calculated to demonstrate the internal consistency of K-HSS.
Results The mean age of the participants was 34.7±9.8 years and 13 (34.2%) were men. K-HSS scores demonstrated a significant positive correlation with serum free thyroxine concentration and decreased significantly with improved thyroid function. K-HSS scores were highest in subclinically thyrotoxic subjects, lower in patients who were euthyroid after treatment, and lowest in the control group at follow-up, but these differences were not significant. Cronbach's α coefficient for the K-HSS was 0.86.
Conclusion The K-HSS is a reliable and valid instrument for evaluating symptoms of thyrotoxicosis in Korean patients.
-
Citations
Citations to this article as recorded by- Effect of thyroid-stimulating hormone suppression on quality of life in thyroid lobectomy patients: interim analysis of a multicenter, randomized controlled trial in low- to intermediate-risk thyroid cancer patients (MASTER study)
Ja Kyung Lee, Eu Jeong Ku, Su-jin Kim, Woochul Kim, Jae Won Cho, Kyong Yeun Jung, Hyeong Won Yu, Yea Eun Kang, Mijin Kim, Hee Kyung Kim, Junsun Ryu, June Young Choi
Annals of Surgical Treatment and Research.2024; 106(1): 19. CrossRef - Effect of increased levothyroxine dose on depressive mood in older adults undergoing thyroid hormone replacement therapy
Jae Hoon Moon, Ji Won Han, Tae Jung Oh, Sung Hee Choi, Soo Lim, Ki Woong Kim, Hak Chul Jang
Clinical Endocrinology.2020; 93(2): 196. CrossRef - Clinical Feasibility of Monitoring Resting Heart Rate Using a Wearable Activity Tracker in Patients With Thyrotoxicosis: Prospective Longitudinal Observational Study
Jie-Eun Lee, Dong Hwa Lee, Tae Jung Oh, Kyoung Min Kim, Sung Hee Choi, Soo Lim, Young Joo Park, Do Joon Park, Hak Chul Jang, Jae Hoon Moon
JMIR mHealth and uHealth.2018; 6(7): e159. CrossRef
- Effect of thyroid-stimulating hormone suppression on quality of life in thyroid lobectomy patients: interim analysis of a multicenter, randomized controlled trial in low- to intermediate-risk thyroid cancer patients (MASTER study)

- Endocrine Research
- Effects of Lobeglitazone, a New Thiazolidinedione, on Osteoblastogenesis and Bone Mineral Density in Mice
- Kyoung Min Kim, Hyun-Jin Jin, Seo Yeon Lee, Hyo Jin Maeng, Gha Young Lee, Tae Jung Oh, Sung Hee Choi, Hak Chul Jang, Soo Lim
- Endocrinol Metab. 2017;32(3):389-395. Published online September 18, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.3.389
- 4,768 View
- 51 Download
- 11 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Bone strength is impaired in patients with type 2 diabetes mellitus despite an increase in bone mineral density (BMD). Thiazolidinedione (TZD), a peroxisome proliferator activated receptor γ agonist, promotes adipogenesis, and suppresses osteoblastogenesis. Therefore, its use is associated with an increased risk of fracture. The aim of this study was to examine the
in vitro andin vivo effects of lobeglitazone, a new TZD, on bone.Methods MC3T3E1 and C3H10T1/2 cells were cultured in osteogenic medium and exposed to lobeglitazone (0.1 or 1 µM), rosiglitazone (0.4 µM), or pioglitazone (1 µM) for 10 to 14 days. Alkaline phosphatase (ALP) activity, Alizarin red staining, and osteoblast marker gene expression were analyzed. For
in vivo experiments, 6-month-old C57BL/6 mice were treated with vehicle, one of two doses of lobeglitazone, rosiglitazone, or pioglitazone. BMD was assessed using a PIXImus2 instrument at the baseline and after 12 weeks of treatment.Results As expected,
in vitro experiments showed that ALP activity was suppressed and the mRNA expression of osteoblast marker genes RUNX2 (runt-related transcription factor 2) and osteocalcin was significantly attenuated after rosiglitazone treatment. By contrast, lobeglitazone at either dose did not inhibit these variables. Rosiglitazone-treated mice showed significantly accelerated bone loss for the whole bone and femur, but BMD did not differ significantly between the lobeglitazone-treated and vehicle-treated mice.Conclusion These findings suggest that lobeglitazone has no detrimental effects on osteoblast biology and might not induce side effects in the skeletal system.
-
Citations
Citations to this article as recorded by- Efficacy and safety of novel thiazolidinedione lobeglitazone for managing type-2 diabetes a meta-analysis
Deep Dutta, Saptarshi Bhattacharya, Manoj Kumar, Priyankar K. Datta, Ritin Mohindra, Meha Sharma
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2023; 17(1): 102697. CrossRef - Efficacy and safety of lobeglitazone, a new Thiazolidinedione, as compared to the standard of care in type 2 diabetes mellitus: A systematic review and meta-analysis
Shashank R. Joshi, Saibal Das, Suja Xaviar, Shambo Samrat Samajdar, Indranil Saha, Sougata Sarkar, Shatavisa Mukherjee, Santanu Kumar Tripathi, Jyotirmoy Pal, Nandini Chatterjee
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2023; 17(1): 102703. CrossRef - A Real-World Study of Long-Term Safety and Efficacy of Lobeglitazone in Korean Patients with Type 2 Diabetes Mellitus
Bo-Yeon Kim, Hyuk-Sang Kwon, Suk Kyeong Kim, Jung-Hyun Noh, Cheol-Young Park, Hyeong-Kyu Park, Kee-Ho Song, Jong Chul Won, Jae Myung Yu, Mi Young Lee, Jae Hyuk Lee, Soo Lim, Sung Wan Chun, In-Kyung Jeong, Choon Hee Chung, Seung Jin Han, Hee-Seok Kim, Ju-Y
Diabetes & Metabolism Journal.2022; 46(6): 855. CrossRef - Comparative Efficacy of Lobeglitazone Versus Pioglitazone on Albuminuria in Patients with Type 2 Diabetes Mellitus
Kyung-Soo Kim, Sangmo Hong, Hong-Yup Ahn, Cheol-Young Park
Diabetes Therapy.2021; 12(1): 171. CrossRef - Lobeglitazone: A Novel Thiazolidinedione for the Management of Type 2 Diabetes Mellitus
Jaehyun Bae, Taegyun Park, Hyeyoung Kim, Minyoung Lee, Bong-Soo Cha
Diabetes & Metabolism Journal.2021; 45(3): 326. CrossRef - Effect of lobeglitazone on motor function in rat model of Parkinson’s disease with diabetes co-morbidity
Kambiz Hassanzadeh, Arman Rahimmi, Mohammad Raman Moloudi, Rita Maccarone, Massimo Corbo, Esmael Izadpanah, Marco Feligioni
Brain Research Bulletin.2021; 173: 184. CrossRef - Comparison of the Effects of Various Antidiabetic Medication on Bone Mineral Density in Patients with Type 2 Diabetes Mellitus
Jeonghoon Ha, Yejee Lim, Mee Kyoung Kim, Hyuk-Sang Kwon, Ki-Ho Song, Seung Hyun Ko, Moo Il Kang, Sung Dae Moon, Ki-Hyun Baek
Endocrinology and Metabolism.2021; 36(4): 895. CrossRef - Xenogeneic native decellularized matrix carrying PPARγ activator RSG regulating macrophage polarization to promote ligament-to-bone regeneration
Xue Han, Lijun Liao, Tian Zhu, Yuchan Xu, Fei Bi, Li Xie, Hui Li, Fangjun Huo, Weidong Tian, Weihua Guo
Materials Science and Engineering: C.2020; 116: 111224. CrossRef - Diabetes pharmacotherapy and effects on the musculoskeletal system
Evangelia Kalaitzoglou, John L. Fowlkes, Iuliana Popescu, Kathryn M. Thrailkill
Diabetes/Metabolism Research and Reviews.2019;[Epub] CrossRef - The effects of diabetes therapy on bone: A clinical perspective
Karim G. Kheniser, Carmen M. Polanco Santos, Sangeeta R. Kashyap
Journal of Diabetes and its Complications.2018; 32(7): 713. CrossRef
- Efficacy and safety of novel thiazolidinedione lobeglitazone for managing type-2 diabetes a meta-analysis

- Clinical Study
- Effect of Pitavastatin Treatment on ApoB-48 and Lp-PLA2 in Patients with Metabolic Syndrome: Substudy of PROspective Comparative Clinical Study Evaluating the Efficacy and Safety of PITavastatin in Patients with Metabolic Syndrome
- Hyo-Sun Lee, Chang Hee Jung, Sung Rae Kim, Hak Chul Jang, Cheol-Young Park
- Endocrinol Metab. 2016;31(1):120-126. Published online March 16, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.1.120
- 3,490 View
- 35 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Apolipoprotein (Apo) B-48 is an intestinally derived lipoprotein that is expected to be a marker for cardiovascular disease (CVD). Lipoprotein-associated phospholipase A2 (Lp-PLA2) is a vascular-specific inflammatory marker and important risk predictor of CVD. The aim of this study was to explore the effect of pitavastatin treatment and life style modification (LSM) on ApoB-48 and Lp-PLA2 levels in metabolic syndrome (MS) patients at relatively low risk for CVD, as a sub-analysis of a previous multi-center prospective study.
Methods We enrolled 75 patients with MS from the PROPIT study and randomized them into two treatment groups: 2 mg pitavastatin daily+intensive LSM or intensive LSM only. We measured the change of lipid profiles, ApoB-48 and Lp-PLA2 for 48 weeks.
Results Total cholesterol, low density lipoprotein cholesterol, non-high density lipoprotein cholesterol, and ApoB-100/A1 ratio were significantly improved in the pitavastatin+LSM group compared to the LSM only group (
P ≤0.001). Pitavastatin+LSM did not change the level of ApoB-48 in subjects overall, but the level of ApoB-48 was significantly lower in the higher mean baseline value group of ApoB-48. The change in Lp-PLA2 was not significant after intervention in either group after treatment with pitavastatin for 1 year.Conclusion Pitavastatin treatment and LSM significantly improved lipid profiles, ApoB-100/A1 ratio, and reduced ApoB-48 levels in the higher mean baseline value group of ApoB-48, but did not significantly alter the Lp-PLA2 levels.
-
Citations
Citations to this article as recorded by- A comprehensive review on the lipid and pleiotropic effects of pitavastatin
Amirhossein Sahebkar, Nasim Kiaie, Armita Mahdavi Gorabi, Massimo R. Mannarino, Vanessa Bianconi, Tannaz Jamialahmadi, Matteo Pirro, Maciej Banach
Progress in Lipid Research.2021; 84: 101127. CrossRef - Change in ALT levels after administration of HMG‐CoA reductase inhibitors to subjects with pretreatment levels three times the upper normal limit in clinical practice
Hyunah Kim, Hyeseon Lee, Tong Min Kim, So Jung Yang, Seo Yeon Baik, Seung‐Hwan Lee, Jae‐Hyoung Cho, Hyunyong Lee, Hyeon Woo Yim, In Young Choi, Kun‐Ho Yoon, Hun‐Sung Kim
Cardiovascular Therapeutics.2018;[Epub] CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Use of Moderate‐Intensity Statins for Low‐Density Lipoprotein Cholesterol Level above 190 mg/dL at Baseline in Koreans
Hun‐Sung Kim, Hyeseon Lee, Sue Hyun Lee, Yoo Jin Jeong, Tong Min Kim, So Jung Yang, Sun Jung Baik, Hyunah Kim, Seung‐Hwan Lee, Jae Hyoung Cho, In‐Young Choi, Kun‐Ho Yoon, Ju Han Kim
Basic & Clinical Pharmacology & Toxicology.2017; 121(4): 272. CrossRef - Another statin option in HIV
Philip E Tarr, Helen Kovari
The Lancet HIV.2017; 4(7): e278. CrossRef - Clinical benefits of pitavastatin: focus on patients with diabetes or at risk of developing diabetes
Vivencio Barrios, Carlos Escobar
Future Cardiology.2016; 12(4): 449. CrossRef
- A comprehensive review on the lipid and pleiotropic effects of pitavastatin

- Clinical Study
- Characterization of Patients with Type 2 Diabetes according to Body Mass Index: Korea National Health and Nutrition Examination Survey from 2007 to 2011
- Dong-Hwa Lee, Kyong Yeun Jung, Kyeong Seon Park, Kyoung Min Kim, Jae Hoon Moon, Soo Lim, Hak Chul Jang, Sung Hee Choi
- Endocrinol Metab. 2015;30(4):514-521. Published online December 31, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.4.514
- 3,601 View
- 42 Download
- 15 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The present study aimed to investigate the clinical characteristics of type 2 diabetes mellitus (T2DM) in Korean adults according to body mass index (BMI) and to analyze the association with cardiovascular disease (CVD).
Methods We conducted a cross-sectional study of data from the Korea National Health and Nutrition Examination Survey from 2007 to 2011. A total of 3,370 patients with T2DM were divided into categories according to BMI. We conducted a comparison of the T2DM patient population composition by BMI category between different countries. We investigated the prevalence of awareness, treatment, and target control of T2DM according to BMI.
Results Patients with T2DM had a higher BMI, and were more likely to have a history of CVD than healthy controls. For Korean adults with T2DM, 8% had BMI ≥30 kg/m2. By contrast, the population of patients with T2DM and BMI ≥30 kg/m2 was 72% in patients in the USA and 56% in the UK. The rate of recognition, treatment, and control has worsened in parallel with increasing BMI. Even in patients with BMI 25 to 29.9 kg/m2, the prevalence of CVD or high risk factors for CVD was significantly higher than in patients with BMI 18.5 to 22.9 kg/m2 (odds ratio, 2.07).
Conclusion Korean patients with T2DM had lower BMI than those in Western countries. Higher BMI was associated with lower awareness, treatment, and control of diabetes, and a positive association was observed between CVD or high risk factors for CVD and BMI, even for patients who were overweight but not obese.
-
Citations
Citations to this article as recorded by- Influenza vaccination trend and related factors among patients with diabetes in Korea: Analysis using a nationwide database
Dong-Hwa Lee, Bumhee Yang, Seonhye Gu, Eung-Gook Kim, Youlim Kim, Hyung Koo Kang, Yeong Hun Choe, Hyun Jeong Jeon, Seungyong Park, Hyun Lee
Frontiers in Endocrinology.2023;[Epub] CrossRef - Diet Quality Scores and Asthenoteratozoospermia Risk: Finding From a Hospital-Based Case–Control Study in China
Qi Cui, Hui-Han Wang, Qi-Jun Wu, Xiao-Bin Wang, Ren-Hao Guo, Xu Leng, Xiao-Ling Tan, Qiang Du, Bo-Chen Pan
Frontiers in Nutrition.2022;[Epub] CrossRef - Obesity definition for personalised treatment of type 2 diabetes Authors’ reply
Ildiko Lingvay, Priya Sumithran, Ricardo V Cohen, Carel W le Roux
The Lancet.2022; 399(10342): 2189. CrossRef - Secular trends and determinants of influenza vaccination uptake among patients with cardiovascular disease in Korea: Analysis using a nationwide database
Min Kim, Bumhee Yang, Seonhye Gu, Eung-Gook Kim, So Rae Kim, Kyeong Seok Oh, Woong-Su Yoon, Dae-Hwan Bae, Ju Hee Lee, Sang Min Kim, Woong Gil Choi, Jang-Whan Bae, Kyung-Kuk Hwang, Dong-Woon Kim, Myeong-Chan Cho, Hyun Lee, Dae-In Lee
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Triglyceride glucose (TyG) index as a predictor of incident type 2 diabetes among nonobese adults: a 12-year longitudinal study of the Korean Genome and Epidemiology Study cohort
Byoungjin Park, Hye Sun Lee, Yong-Jae Lee
Translational Research.2021; 228: 42. CrossRef - Gamitaeeumjowee-Tang for weight loss in diabetic patients: A retrospective chart review
A-Reum Lee, Da-Yeon Lee, Min-Ji Kim, Hyang-Sook Lee, Ka-Hye Choi, Seo-Young Kim, Young-Woo Lim, Young-Bae Park
Journal of Korean Medicine.2021; 42(1): 46. CrossRef - Effect of cilostazol, a phosphodiesterase‐3 inhibitor, on coronary artery stenosis and plaque characteristics in patients with type 2 diabetes: ESCAPE study
Dong‐Hwa Lee, Eun Ju Chun, Tae Jung Oh, Kyoung Min Kim, Jae Hoon Moon, Sung Hee Choi, Kyong Soo Park, Hak Chul Jang, Soo Lim
Diabetes, Obesity and Metabolism.2019; 21(6): 1409. CrossRef - The Differential Role of Vitamin D in Type 2 Diabetes Management and Control in Minority Populations
Miyong To Kim, Kim Byeng Kim, Jisook Ko, Nicole Murry, David Levine, Ju-Young Lee
Journal of Immigrant and Minority Health.2019; 21(6): 1266. CrossRef - House dust mite and Cockroach specific Immunoglobulin E sensitization is associated with diabetes mellitus in the adult Korean population
Mee Kyoung Kim, Jee Sun Jeong, Kyungdo Han, Ki Hyun Baek, Ki-Ho Song, Hyuk-Sang Kwon
Scientific Reports.2018;[Epub] CrossRef - Long‐term effects on glycaemic control and β‐cell preservation of early intensive treatment in patients with newly diagnosed type 2 diabetes: A multicentre randomized trial
Suk Chon, Sang Youl Rhee, Kyu Jeung Ahn, Sei Hyun Baik, Yongsoo Park, Moon Suk Nam, Kwan Woo Lee, Soon Jib Yoo, Gwanpyo Koh, Dae Ho Lee, Young Seol Kim, Jeong‐Taek Woo
Diabetes, Obesity and Metabolism.2018; 20(5): 1121. CrossRef - Association between Body Weight Changes and Menstrual Irregularity: The Korea National Health and Nutrition Examination Survey 2010 to 2012
Kyung Min Ko, Kyungdo Han, Youn Jee Chung, Kun-Ho Yoon, Yong Gyu Park, Seung-Hwan Lee
Endocrinology and Metabolism.2017; 32(2): 248. CrossRef - Abnormal subchondral bone remodeling and its association with articular cartilage degradation in knees of type 2 diabetes patients
Yan Chen, Yong-Can Huang, Chun Hoi Yan, Kwong Yuen Chiu, Qingjun Wei, Jingmin Zhao, X Edward Guo, Frankie Leung, William W Lu
Bone Research.2017;[Epub] CrossRef - Social Networking Services-Based Communicative Care for Patients with Diabetes Mellitus in Korea
Hun-Sung Kim, Yoo Jeong, Sun Baik, So Yang, Tong Kim, Hyunah Kim, Hyunyong Lee, Seung-Hwan Lee, Jae Cho, In-Young Choi, Kun-Ho Yoon
Applied Clinical Informatics.2016; 07(03): 899. CrossRef - Pharmacological Management of Obesity in Patients with Type 2 Diabetes: An Update
Eun Ju Lee, Tae Nyun Kim
The Korean Journal of Obesity.2016; 25(3): 121. CrossRef - Response: Characterization of Patients with Type 2 Diabetes according to Body Mass Index: Korea National Health and Nutrition Examination Survey from 2007 to 2011 (Endocrinol Metab 2015;30:514-21, Dong-Hwa Lee et al.)
Sung Hee Choi
Endocrinology and Metabolism.2016; 31(2): 347. CrossRef - Letter: Characterization of Patients with Type 2 Diabetes according to Body Mass Index: Korea National Health and Nutrition Examination Survey from 2007 to 2011 (Endocrinol Metab 2015;30:514-21, Dong-Hwa Lee et al.)
Eun-Hee Cho
Endocrinology and Metabolism.2016; 31(2): 345. CrossRef
- Influenza vaccination trend and related factors among patients with diabetes in Korea: Analysis using a nationwide database

- A Case of Ectopic ACTH Syndrome Associated with Metastatic Prostate Cancer.
- Eun Ky Kim, Soo Heon Kwak, Hwa Young Ahn, Ah Reum Khang, Hyo Jin Park, So Yeon Park, Sang Eun Lee, Hak Chul Jang, Seong Yeon Kim, Young Joo Park
- Endocrinol Metab. 2012;27(3):237-243. Published online September 19, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.3.237
- 1,803 View
- 26 Download
-
 Abstract
Abstract
 PDF
PDF - Ectopic adrenocorticotropic hormone (ACTH) syndrome is mostly associated with neuroendocrine tumors and small cell carcinoma of the lung. This syndrome of prostate cancer is rare and has been reported in only a few cases. We report a patient with ectopic ACTH production associated with metastatic prostate cancer. A 70-year-old patient with metastatic prostate cancer was admitted to our hospital with septic shock. He had a history of hormonal therapy and transurethral prostatectomy. Adrenocortical function was checked due to consistent fever and poor general condition, which revealed markedly increased levels of basal plasma ACTH and serum cortisol. The patient did not present typical signs of the Cushing's syndrome, however, hypokalemia and a history of hypertension were found. He died in days as a result of multi-organ failure. On pathology, the prostatectomy specimen showed a tumor composed of mixed populations of adenocarcinoma and small cell carcinoma. The tumor cells in the small cell component were positive for chromogranin and ACTH. Although neuroendocrine differentiation in prostate cancer is rare, etopic ACTH production should be considered in patients with prostate cancer as well as in clinical features of ACTH hypersecretion.

- Clinical Characteristics of Langerhans Cell Histiocytosis with Hypothalamo-Pituitary Involvement.
- Eun Shil Hong, Jung Hun Ohn, Jung Hee Kim, Yul Hwang-Bo, Jin Joo Kim, Jung Hee Kwon, Jung Won Lee, Se Youn Choi, Eun Kyung Lee, Sun Wook Cho, Chan Soo Shin, Kyong Soo Park, Hak Chul Jang, Bo Youn Cho, Hong Kyu Lee, Choong Ho Shin, Sei Won Yang, Seong Yeon Kim
- Endocrinol Metab. 2011;26(1):38-43. Published online March 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.1.38
- 1,940 View
- 23 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Langerhans cell histiocytosis (LCH) is a rare disease that involves a clonal proliferation of Langerhans cells. LCH has a predilection for hypothalamo-pituitary axis (HPA) dysfunction, and this leads to diabetes insipidus (DI) and/or anterior pituitary dysfunction. Here, we describe the endocrine dysfunction and clinical characteristics of adult patients with LCH and we analyzed the differences between an adult-onset type and a childhood-onset type. METHODS: The data was obtained from a retrospective chart review of the patients with LCH that involved the HPA and who attended Seoul National University Hospital. The patients were classified into the adult-onset type (age at the time of diagnosis > or = 16) and the childhood-onset type (age at the time of diagnosis < or = 15). RESULTS: Ten patients (9 males and 1 female) were diagnosed with LCH involving the HPA. Five patients were classified as an adultonset type and the other five patients were classified as a childhood-onset type. The median follow-up duration was 6 (3-12) years for the adult-onset type and 16 (15-22) years for the childhood-onset type. All the patients presented with DI as the initial manifestation of HPA involvement. Four adult-onset patients and three childhood-onset patients had a multi-system disease. Panhypopituitarism developed in three adult-onset patients and in one childhood-onset patient. The pituitary lesion of the three adult-onset patients had spread to the brain during the follow-up duration. In contrast, the pituitary lesion of the other two adult-onset patients without panhypopituitarism and all the childhood-onset patients had not changed. CONCLUSION: DI was the initial presentation symptom of HPA involvement. Anterior pituitary hormone deficiency followed in some patients. Compared with the childhood-onset patients, the adult-onset patients were more likely to have panhypopituitarism and a poor prognosis. -
Citations
Citations to this article as recorded by- Pulmonary Langerhans Cell Histiocytosis in an Adult Male Presenting with Central Diabetes Insipidus and Diabetes Mellitus: A Case Report
Yeun Seoung Choi, Jung Soo Lim, Woocheol Kwon, Soon-Hee Jung, Il Hwan Park, Myoung Kyu Lee, Won Yeon Lee, Suk Joong Yong, Seok Jeong Lee, Ye-Ryung Jung, Jiwon Choi, Ji Sun Choi, Joon Taek Jeong, Jin Sae Yoo, Sang-Ha Kim
Tuberculosis and Respiratory Diseases.2015; 78(4): 463. CrossRef - Adult Multisystem Langerhans Cell Histiocytosis Presenting with Central Diabetes Insipidus Successfully Treated with Chemotherapy
Jung-Eun Choi, Hae Ri Lee, Jung Hun Ohn, Min Kyong Moon, Juri Park, Seong Jin Lee, Moon-Gi Choi, Hyung Joon Yoo, Jung Han Kim, Eun-Gyoung Hong
Endocrinology and Metabolism.2014; 29(3): 394. CrossRef
- Pulmonary Langerhans Cell Histiocytosis in an Adult Male Presenting with Central Diabetes Insipidus and Diabetes Mellitus: A Case Report

- Pituitary Apoplexy in Korea - Characteristics, Treatment Options and Outcomes.
- Jung Ah Lim, Jin Taek Kim, Min Joo Kim, Tae Hyuk Kim, Yenna Lee, Hwa Young Cho, Chan Soo Shin, Kyong Soo Park, Hak Chul Jang, Bo Youn Cho, Hong Kyu Lee, Seong Yeon Kim
- J Korean Endocr Soc. 2009;24(4):247-253. Published online December 1, 2009
- DOI: https://doi.org/10.3803/jkes.2009.24.4.247
- 2,076 View
- 23 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Reports on pituitary apoplexy in Korea are limited. There are two treatment options for pituitary apoplexy - surgical decompression and conservative management. In this study, we examined clinical presentation and outcomes following different therapies in Korean patients with pituitary apoplexy. METHODS: Clinical data and treatment outcomes from 52 patients with pituitary apoplexy who visited Seoul National University Hospital between January 1992 and June 2008 were reviewed retrospectively. Patients were divided into 2 groups according to management options (a surgery group vs. a conservative management group) and their outcomes were compared. For patients who underwent surgery due to neurological symptoms, outcomes were compared between early and late surgery groups. RESULTS: Headache (73.1%) was the most common presenting symptom, and more than half of the patients were reported to have visual symptoms. The most common type of pathology was a nonfunctioning pituitary adenoma (67.3%). Nine patients received conservative management and 43 underwent surgical decompression. Their recovery from neurological and endocrinological abnormalities were similar. Among patients who showed neurological symptoms, 9 underwent surgery within 1 week of symptom onset and 24 underwent surgery after 1 week. There was no significant difference between outcomes of early and late surgery groups except recovery from impaired visual deficit was greater in the late surgery group. CONCLUSION: Patients with pituitary apoplexy in Korea show similar clinical features as similar patients in other countries. In our study, there was no significant difference between clinical outcomes of the surgery group and the conservative treatment group. -
Citations
Citations to this article as recorded by- The Outcomes of Pituitary Apoplexy with Conservative Treatment: Experiences at a Single Institution
Youngbeom Seo, Yong Hwy Kim, Yun-Sik Dho, Jung Hee Kim, Jin Wook Kim, Chul-Kee Park, Dong Gyu Kim
World Neurosurgery.2018; 115: e703. CrossRef - Characteristics and Treatment Options of Pituitary Apoplexy
Dong-Sun Kim
Journal of Korean Endocrine Society.2009; 24(4): 237. CrossRef
- The Outcomes of Pituitary Apoplexy with Conservative Treatment: Experiences at a Single Institution

- Discrepancy between the Growth Hormone and Insulin-like Growth Factor-I Concentrations in Patients with Acromegaly.
- Ji Won Yoon, Mi Yeon Kang, Hwa Young Ahn, Jee Hyun An, Sang Wan Kim, Chan Soo Shin, Kyong Soo Park, Hak Chul Jang, Bo Youn Cho, Hong Kyu Lee, Seong Yeon Kim
- J Korean Endocr Soc. 2008;23(6):395-403. Published online December 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.6.395
- 1,865 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
This study was performed to evaluate the frequency and clinical characteristics of patients with active acromegaly and who show discordance of the growth hormone (GH) level and the insulin-like growth factor-I (IGF-I) level. METHODS: We reviewed the medical records of the patients who were diagnosed with acromegaly between 01/01/1995 and 6/30/2007 at Seoul National University Hospital. We selected only the patients whose basal GH and IGF-I levels were available. We investigated the pre- and post-operative clinical characteristics, as well as the blood concentrations of GH and IGF-I. The concordance rate between the two hormones was examined. The patients were considered to have active disease on the basis of their IGF-I levels above the normal range, after adjustment for age and gender, and their mean basal GH value was > or = 2.5 microgram/L. The hormone levels and the clinical parameters were compared between the hormone concordant and discordant groups. RESULTS: We reviewed the preoperative records of 103 acromegalic patients, and these patients met the above-mentioned criteria. 53 postoperative patients who were not cured by operation were monitored without them receiving radiation or medical therapy. Both the basal GH and IGF-I levels were above normal in 103 patients preoperatively, and the discordant rate was 0% (0/103 cases). Postoperatively, the discordant rate between the two hormones was increased to 30.2% (16/53 cases). Age, gender, body mass index and tumor size were insignificantly different between the concordant and discordant groups. However, postoperative residual tumors were less frequently observed in the discordant group (P = 0.006). CONCLUSION: For the patients with acromegaly, unlike the 0% discordance preoperatively, 30.2% of patients showed a discrepancy between their GH and IGF-I levels postoperatively. The patients who had hormonal discrepancy were less likely to have residual tumors after operation. Considering the frequency of this hormonal discrepancy, both hormone levels should be measured to evaluate the disease activity after treatment. Further, oral glucose tolerance testing should be performed and especially for the patients with an increased GH level, but who have a normal IGF-I concentration.

- The Effects on Visceral Fat and Cardiovascular Risk Factors of Testosterone Replacement in Secondary Hypogonadal Men.
- Eui Sil Hong, Sung Yeon Kim, Young Ju Choi, Sang Wan Kim, Chan Soo Shin, Kyong Soo Park, Hak Chul Jang, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee
- J Korean Endocr Soc. 2005;20(3):252-260. Published online June 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.3.252
- 1,847 View
- 19 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Increased body fat, abdominal obesity and insulin resistance are important clinical features in hypogonadal men. Several studies have demonstrated that a low testosterone concentration in men is associated with coronary heart disease, visceral obesity and insulin resistance. In this study, the effects of testosterone replacement therapy on the abdominal visceral fat and cardiovascular risk factors in hypogonadal men were investigated. METHODS: We selected 26 men with secondary hypogonadism (mean serum testosterone+/-SD 0.39+/- 0.57ng/mL), who were then treated with testosterone for 12 months. We measured the body composition, including the abdominal visceral fat area by abdominal CT at the L4 level, both before and 12 months after treatment, and the lipid profile, fasting plasma insulin, HOMA-IR and the serum homocysteine, CRP and IL-6 before and 6, 12 months after treatment. RESULTS: With respect to the body composition, the lean body mass had significantly increased 12 months after treatment(P= 0.002), but there were no significant changes in the body fat mass and abdominal visceral fat area. There was a trend toward a decreased fasting plasma insulin and HOMA-IR, but this did not reach statistical significance. The total cholesterol had decreased significantly at 12 months(P=0.04) and the HDL cholesterol decreased significantly over the course of study(P=0.02). There were no significant changes in the serum homocysteine, CRP and IL-6 after treatment. CONCLUSIONS: After 12 months testosterone replacement therapy in the 26 men with hypogonadism, the lean body mass had increased significantly, but there was no significant change on the abdominal visceral fat during the treatment period. Testosterone replacement had deleterious effect on HDL cholesterol, but not significant effects on insulin resistance and the serum homocysteine, CRP and IL-6. These results suggest that testosterone replacement therapy may have a few adverse effects on cardiovascular diseases in hypogonadal men. However, it will be necessary to examine the long-term effects of testosterone replacement on the incidence of cardiovascular events as well as the cardiovascular risk factors in men with hypogonadism -
Citations
Citations to this article as recorded by- The Association of Level of Testosterone and Parameters of Obesity
Chong Hwa Kim
The Korean Journal of Obesity.2015; 24(1): 28. CrossRef - The Relationship between Various Obesity Indices and Level of Male Hormone according to Different Age Groups
Yoo-Jung Lee, Hyeon-Ju Kim, Mi-Hee Kong
The Korean Journal of Obesity.2014; 23(4): 245. CrossRef - Androgen Receptor Gene CAG Repeat Polymorphism and Effect of Testosterone Therapy in Hypogonadal Men in Korea
Min Joo Kim, Jin Taek Kim, Sun Wook Cho, Sang Wan Kim, Chan Soo Shin, Kyong Soo Park, Seong Yeon Kim
Endocrinology and Metabolism.2011; 26(3): 225. CrossRef - Effects of Androgen on the Cardiovascular System in the Aging Male
Jin Wook Kim, Je Jong Kim, Du Geon Moon
Korean Journal of Andrology.2011; 29(1): 10. CrossRef
- The Association of Level of Testosterone and Parameters of Obesity

- High-Dose Hook Effect in Patients with Macroprolactinoma.
- Sung Yeon Kim, Chul Gu Park, Young Ju Choi, Eui Sil Hong, Sang Wan Kim, Chan Soo Shin, Hak Chul Jang, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee
- J Korean Endocr Soc. 2005;20(2):148-153. Published online April 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.2.148
- 1,978 View
- 20 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Large amounts of antigen may produce false low values on immunoradiometric assays due to the so-called high-dose hook effect. The physicians' awareness of the possibility of the "high-dose hook effect" will prevent preoperative misdiagnosis. The study was designed to identify the frequency and clinical features of patients with pituitary macroadenomas in whom a high-dose PRL hook effect was documented. METHODS: Our retrospective study involved 42 patients with non-functioning pituitary adenomas (tumor diameter >30mm) who underwent transsphenoidal microsurgery from between Jan 1999 to Aug 2004, and 6 patients with non-functioning pituitary adenoma(tumor diameter>30mm) were selected for prospective study from Sep 2003 to Feb 2004. Our retrospective study also involved 13 patients with macroprolactinoma for the comparison of the clinical features. RESULTS: 1) The presence of a high-dose hook effect was retrospectively suggested when the PRL levels increased in 4 out of the 42 patients with non- functioning adenomas(tumor diameter >30mm) after surgery. Post-operative immunohistochemical staining of their pituitary specimens revealed the tumors to be prolactinoma. 2) Prospectively, dilution testing of the specimens obtained before surgery was done in the 6 patients, and one patient presented with a case of the hook effect. The patient's prolactin level was measured at 53.1ng/mL before dilution and this was increased up to 22,600ng/mL upon the 1:1000 dilution. 3) Conclusively, the hook effect was seen in 5 of the 48 patients(10.4%) with non-functioning pituitary adenoma(tumor diameter >30mm) 4) Compared with other 2 patient groups(the macroprolactinoma(N=13) group, and the non-functioning pituitary tumor(N=43) group), the high-dose PRL hook effect is more likely to be observed in male patients with large pituitary tumors. CONCLUSION: In order to avoid the high-dose hook effect, PRL should be assayed at 1:100~1:200 or even higher dilutions of serum from all patients(and especially the male patients) with large pituitary tumors -
Citations
Citations to this article as recorded by- Multiple Endocrine Neoplasia Type 1 Presenting with an Invasive Giant Prolactinoma
Jinhoon Cha, Jin Seo Kim, Jung Suk Han, Yeon Won Park, Min Joo Kim, Yun Hyi Ku, Hong Il Kim
The Korean Journal of Medicine.2016; 91(3): 300. CrossRef
- Multiple Endocrine Neoplasia Type 1 Presenting with an Invasive Giant Prolactinoma

- The Postpartum Recurrence of Graves'Disease and its Contributing Factors.
- Chang Hoon Yim, Hyun Ah Choi, Seung Suk Han, Hae Sung Kim, Chang Uk Lee, Ho Yeon Chung, Ki Ok Han, Hak Chul Jang, Won Keun Park, Hyun Ku Yoon, In Kwon Han
- J Korean Endocr Soc. 2002;17(2):189-196. Published online April 1, 2002
- 1,157 View
- 32 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Pregnancy affects the course of Graves' Disease (GD), and patients who initially maintain euthyroid function into their middle trimester with minimum doses of antithyroid drugs become exacerbated after delivery. Even patients who are completely cured, requiring no treatment during pregnancy, can relapse after delivery. In this study, we examined the postpartum changes in the thyroid functions of patients with GD, and attempted to determine the factors contributing to these changes. METHODS: The study subjects were recruited from pregnant women visiting our outpatient clinic for routine prenatal evaluations. 45 women previously diagnosed with GD, who had been treated and cured with hyperthyroidism, and were no longer taking any thyroid medications, were evaluated for 1 year post delivery. RESULTS: Among 45 patients, 20 (44.4%) developed thyroid disorders following delivery. Postpartum thyroiditis (PPT) developed in 8 patients (17.8%), and GD developed in 12 (26.0%). The onset of the PPT disease 3.1 +/- 1.4 months following delivery, which was significantly earlier than the 6.7 +/- 2.7 months required for the post delivery onset of GD (p=0.003). The TBII values, measured during the thyrotoxic state in each womaen, were negative in women with PPT and positive in 71.4% of women with GD (p=0.030). The duration of treatment for hyperthyroidism prior or pregnancy, the number of recurrences, and the time interval without treatment, were not associated with the development of postpartum thyroid disorders. Whereas, the mean number of past pregnancies for women who developed PPT was 3.9 +/- 2.1, and was significantly higher than the 2.2+/- 1.7 for women developing no thyroid dysfunctions (p=0.044). In 13 women their initial onset of GD occurred within one year postpartum, 7 (53.8%) having had a recurrence, which was significantly higher than in women whose disease onset occurred unrelated to delivery (5 of 32 women: 15.6%). CONCLUSION: Women with GD developed postpartum thyroid dysfunctions in 44.4% of cases. Women whose initial disease onset occurred within one year postpartum had higher recurrences of GD, and women who developed PPT had a history of higher gravidity compared to the euthyroid women postpartum. Therefore, if women with GD develop postpartum thyroid dysfunctions, the diagnosis should be made, and a treatment modality planned, following careful considerations of the patients' past obstetric history, changes in clinical manifestations and the TBII values.


 KES
KES

 First
First Prev
Prev



